📋 Key Information Summary
- Definition: Carpal Tunnel Syndrome (CTS) is a common compressive neuropathy caused by increased pressure on the median nerve within the carpal tunnel.
- Epidemiology: Affects 3-6% of adults in Australia; more common in women, dominant hand, and with increasing age.
- Key Risk Factors: Female sex, pregnancy, obesity, diabetes mellitus, hypothyroidism, rheumatoid arthritis, and repetitive wrist movements.
- Diagnosis: Primarily clinical, supported by characteristic symptoms (nocturnal paraesthesia, hand clumsiness) and provocative tests (Tinel's, Phalen's). Nerve conduction studies (NCS) confirm diagnosis and quantify severity.
- First-Line Management: Conservative measures including nocturnal wrist splints and activity modification.
- Pharmacotherapy: Ultrasound-guided corticosteroid injection (e.g., methylprednisolone) provides short-to-medium term symptom relief. Not a definitive cure.
- Referral for NCS: Indicated for diagnostic uncertainty, failed conservative treatment, or when surgery is considered. MBS item 11000 (standard) or 11003 (with F-wave) available.
- Surgical Indications: Persistent symptoms despite conservative therapy, thenar muscle atrophy/wasting, or severe NCS findings.
- Surgical Options: Open or endoscopic carpal tunnel release. Both are effective; choice depends on surgeon expertise and patient factors.
- Special Populations: Pregnancy-related CTS often resolves postpartum. Manage conservatively. In diabetes and rheumatoid arthritis, treat underlying condition concurrently.
- ATSI Considerations: Higher prevalence of diabetes and obesity may increase CTS risk. Ensure equitable access to specialist and surgical services.
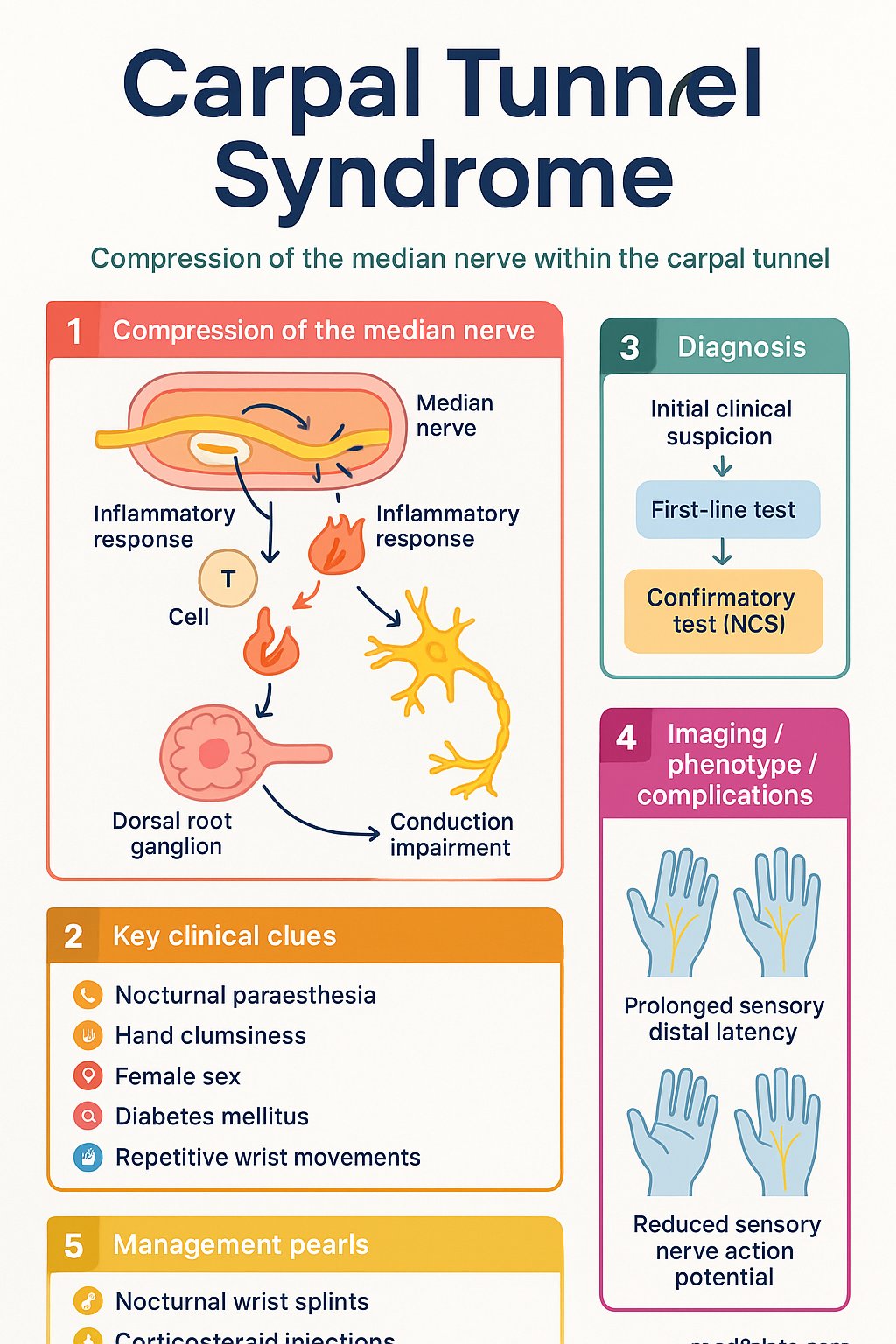
Introduction & Australian Epidemiology
Carpal Tunnel Syndrome (CTS) is the most common entrapment neuropathy, resulting from compression of the median nerve as it passes through the rigid carpal tunnel in the wrist. It is a significant cause of hand pain, numbness, and functional impairment in the working-age population.
In Australia, CTS has a lifetime prevalence estimated at 3-6%. It disproportionately affects women (female-to-male ratio approximately 3:1), with peak incidence between ages 40 and 60. Data from the Australian Institute of Health and Welfare (AIHW) indicates CTS as a leading cause of work-related musculoskeletal disorder, particularly in occupations involving repetitive wrist flexion, forceful grip, and vibration exposure. The condition imposes a substantial burden through lost productivity, healthcare utilisation, and workers' compensation claims.
Median Nerve Anatomy & Risk Factors
Anatomy
The carpal tunnel is a narrow, osteofibrous passageway located at the volar aspect of the wrist. Its boundaries are the carpal bones (floor and walls) and the transverse carpal ligament (flexor retinaculum) forming the roof. The tunnel contains nine digital flexor tendons and the median nerve. The median nerve provides sensory innervation to the palmar aspects of the lateral 3½ fingers (thumb, index, middle, radial half of ring finger) and motor innervation to the thenar muscles (opponens pollicis, abductor pollicis brevis, superficial head of flexor pollicis brevis).
Risk Factors
Risk factors increase the volume of contents within the tunnel or decrease the size of the tunnel itself.
| Category | Specific Factors |
|---|---|
| Anatomical | Female sex (smaller tunnel cross-section), wrist fractures (Colles'), dislocations, acromegaly |
| Physiological / Hormonal | Pregnancy, menopause, hypothyroidism, renal failure (dialysis amyloidosis), obesity |
| Inflammatory / Systemic | Rheumatoid arthritis, gout, diabetes mellitus (endoneurial oedema) |
| Occupational / Activity | Repetitive wrist flexion/extension, forceful grip, use of vibrating tools (controversial but frequently cited) |
Clinical Assessment
Diagnosis is primarily clinical, based on characteristic history and examination findings.
History
- Symptoms: Numbness, tingling (paraesthesia), burning pain in the median nerve distribution. Often worse at night or with activities like driving, reading, or holding a phone.
- Nocturnal Symptoms: A hallmark feature. Patients may report waking with a "dead hand" needing to shake or wring it to relieve symptoms.
- Clumsiness: Difficulty with fine motor tasks (buttons, dropping objects) due to sensory loss or thenar weakness.
Physical Examination
- Sensory: Test light touch and two-point discrimination over the median nerve territory. Check for sensory deficit.
- Motor: Assess thumb opposition and abduction strength. Look for thenar muscle flattening (atrophy) in advanced cases.
- Provocative Tests:
- Tinel's Sign: Tapping over the carpal tunnel at the wrist. A positive test reproduces paraesthesia in the median nerve distribution. Sensitivity ~50%, Specificity ~77%.
- Phalen's Test: Patient holds wrists in full flexion for 60 seconds. A positive test reproduces symptoms. Sensitivity ~68%, Specificity ~73%.
- Carpal Tunnel Compression Test: Direct pressure over the carpal tunnel for 30 seconds. High sensitivity (~89%).
Nerve Conduction Studies (NCS)
Nerve conduction studies (NCS) and electromyography (EMG) are the gold standard for confirming the diagnosis of CTS, localising the lesion, and grading its severity. They are crucial when the diagnosis is uncertain, symptoms are severe, or surgical intervention is planned.
Role and Indications
- Diagnostic Confirmation: Differentiates CTS from mimics like cervical radiculopathy or generalised polyneuropathy.
- Severity Grading: Guides prognosis and treatment choices (e.g., mild CTS may respond to splints; severe CTS may require surgery).
- Surgical Planning: Provides objective baseline data and confirms the diagnosis prior to decompression.
Key Findings in CTS
- Sensory: Prolonged sensory distal latency and reduced sensory nerve action potential (SNAP) amplitude across the wrist.
- Motor: Prolonged motor distal latency and reduced compound muscle action potential (CMAP) amplitude (in severe cases).
- Comparative Studies: Comparing median nerve latency to ulnar or radial latencies in adjacent fingers increases diagnostic sensitivity.
Australian Access & MBS
NCS are performed by neurologists, rehabilitation specialists, or suitably trained technicians. They are available in major public hospitals and private neurophysiology practices.
Ultrasound Diagnosis
High-resolution ultrasound (US) is a non-invasive, cost-effective, and dynamic imaging modality for evaluating CTS. It serves as an excellent adjunct to clinical examination and NCS.
Diagnostic Criteria
- Cross-Sectional Area (CSA): The most reliable measure. A CSA of the median nerve >10-12 mm² at the carpal tunnel inlet (pisiform level) is highly suggestive of CTS.
- Flattening Ratio: Increased ratio of the nerve's anteroposterior to transverse diameter within the tunnel.
- Bowing of the Flexor Retinaculum: Indicates increased carpal tunnel pressure.
- Nerve Vascularity: Increased intraneural vascularity (hyperaemia) on colour Doppler may be present in active inflammation.
Advantages & Limitations
- Dynamic assessment (e.g., during wrist movement).
- Visualises anatomical variants, ganglion cysts, or tenosynovitis as causes.
- Guides accurate steroid injections.
- No radiation, well-tolerated, quick.
- Operator-dependent.
- Does not provide functional/physiological data like NCS (e.g., conduction velocity).
- Less useful for assessing severity in advanced neuropathy with axonal loss.
Ultrasound is particularly useful when NCS are unavailable, contraindicated, or when an alternative structural cause is suspected. It is increasingly used in Australian rheumatology and sports medicine practices.
